What is Pelvic Congestion Syndrome?
 It is estimated that more than a third of all women will experience chronic pelvic pain during their lifetime. Chronic pelvic pain is defined as pain lasting greater than six months.
It is estimated that more than a third of all women will experience chronic pelvic pain during their lifetime. Chronic pelvic pain is defined as pain lasting greater than six months.
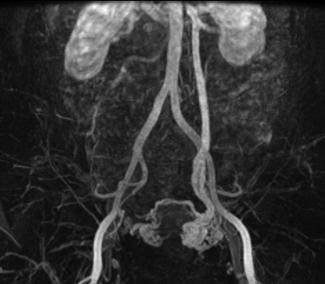
A multidisciplinary team approach is needed to diagnose and treat this often complex medical condition. After a physical examination, a Pap test, and routine laboratory bloodwork, an ultrasound, CT or MRI may be obtained rule out other significant pelvic pathology. If the clinical symptoms are those of chronic pelvic pain, worse when sitting or standing, relieved with lying down, the possibility of dilated ovarian veins and pelvic varices causing these symptoms must be considered.
Chronic pelvic pain caused by reflux or obstruction of the gonadal, gluteal, or periuterine veins is called pelvic congestion syndrome. Incompetent venous valves in the ovarian veins can lead to reflux and development of pelvic varices.These dilated veins may sometimes be seen with ultrasound, CT, or MRI. These enlarged and abnormal veins are more common on the left, more likely in women who have had multiple pregnancies, and very similar in cause to lower extremity varicose veins.
How common is Pelvic Congestion Syndrome?
It is estimated that approximately 30 percent of patients with chronic pelvic pain suffer from pelvic congestion syndrome as the sole cause and an additional 15 percent have pelvic congestion syndrome with at least one additional cause of pelvic pain.
How is Pelvic Congestion Syndrome treated?
Chronic pelvic pain due to ovarian and pelvic varices (varicose veins) is treated using nonsurgical, minimally invasive, transcatheter techniques. The procedure is performed under conscious sedation and the patient is usually awake. General anesthesia is not required. The procedure usually takes less than one hour.
How should I prepare for the procedure?
Before the procedure, you may have blood tested to determine how well your kidneys and your blood clotting are functioning. You should inform your doctor of all medications you are taking, including any herbal supplements. Inform us of any allergies, particularly to local or general anesthetic medications or to contrast materials (sometimes called X-ray dye) or to latex gloves. Always inform your doctor if you are or may be pregnant.
Eat a light meal the evening before. You will be instructed not to eat or drink after midnight before the procedure, and if you are diabetic you should receive instructions from your doctor about adjusting medications and insulin dose on the day of the procedure. You will be asked to remove your clothing and wear a gown during the procedure. You will also need a ride home with a friend or relative.
How is the procedure performed and when will I get my results?
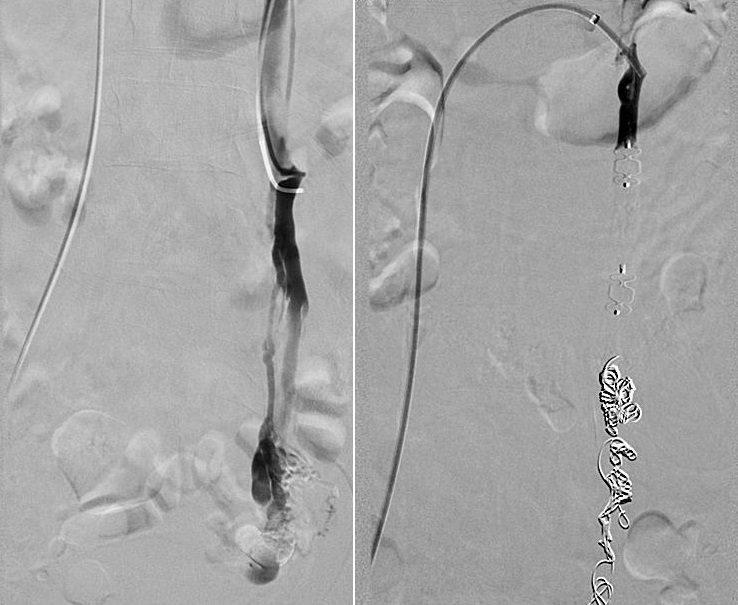 First, the diagnosis of ovarian varices is confirmed by placing a small catheter through the large vein in the groin and into specific veins. If varices are found they can be treated at the same time. The blood supply to the enlarged veins causing the symptoms is blocked by the use of coils and embolic agents.
First, the diagnosis of ovarian varices is confirmed by placing a small catheter through the large vein in the groin and into specific veins. If varices are found they can be treated at the same time. The blood supply to the enlarged veins causing the symptoms is blocked by the use of coils and embolic agents.
Regarding ovarian and pelvic varices, the procedure may be performed in two stages. Once the ovarian varices are treated, if there are additional pelvic varices, these are usually treated at a later time. The second half of the embolization procedure may be performed days to weeks later if the patient’s symptoms do not improve.
The interventional radiologist will be able to inform you whether the procedure was technically successful. The interventional radiologist may consider treating any additional pelvic varices if your symptoms do not improve in two to three months.
What is the recovery like?
The recovery time for women who undergo embolization of ovarian and pelvic varices is similar. Both procedures are usually performed on an outpatient basis. The patient may require mild oral pain medications for relief of discomfort after the procedure. Pain is most significant during the first three days.
Most women resume light activities two to three days after the procedure and most patients are able to resume their normal level of activity in five to ten days.
How effective is ovarian vein embolization for Pelvic Congestion Syndrome and what are the risks?
Ovarian vein embolization and treatment of pelvic varices are very effective procedures. On average, 85 to 95 percent of patients experience significant or total relief of their symptoms. Most women report symptom relief within the first few days after the procedure. Symptoms may recur in up to 5 to 8 percent of patients, usually due to additional pelvic varices that can be treated with a second procedure.
Some patients (<5 percent) may report mild fever or flank discomfort. Venipuncture site hematoma and coil migration are very rare.
Radiologyinfo.org for Patients
The radiology information resource for patients. RadiologyInfo.org tells you how various X-ray, CT, MRI, ultrasound, radiation therapy and other procedures are performed. It also addresses what you may experience and how to prepare for the exams. The website contains over 200 procedure, exam and disease descriptions covering diagnostic and interventional radiology, nuclear medicine, radiation therapy and radiation safety and is updated frequently with new information. All material on the RadiologyInfo.org website is reviewed and approved by experts in the field of radiology from the ACR and RSNA, as well as other professional radiology organizations.
